The cost of anholistic care
Being 'holistic' in care delivery can seem anachronistic, paying homage to new age thinking and practices. Paradoxically, being holistic in nursing can also mimic an admin exercise that amounts to ticking the boxes. So for Hodges' model - have you visited all the care domains?
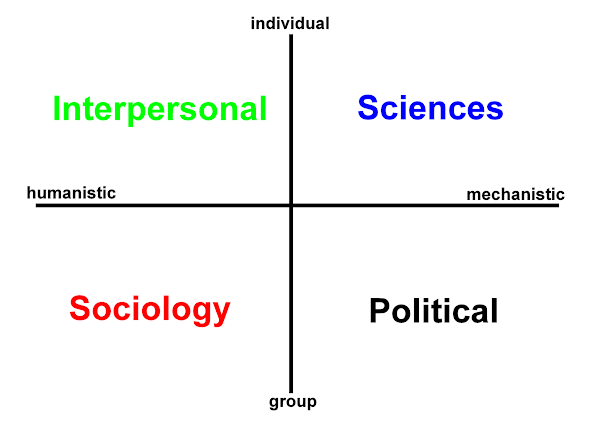
- INTERPERSONAL care ✓
- POLITICAL care ✓
- PHYSICAL care ✓
- SOCIAL care ✓
- idealised care;
- standardised care;
- evidence of policy, targets;
- sign posting for the care pathway;
- an essential care aspiration that emphasizes the individual's strengths and resources.
Last month 23 June, 2010 The Guardian, Society Guardian featured The high cost of return:
Hospitals could lose up to £1.5bn of NHS funding a year because of the government's decision to penalise those where patients return within 30 days of being treated. That is the conclusion of research conducted by health analysts Dr Foster into the potential impact of the tough new policy. It warns that NHS trusts face large potential losses, the biggest could reach £28.7m, as a result of the new approach. In all, 146 acute, specialist and mental health trusts could lose out. Denis Campbell, p.3.Apparently -
Andrew Lansley wants to force the NHS to provide better care in hospitals and mental health establishments, to keep treating patients there until they are fit to leave and to work more closely with community-based healthcare professionals, such as GPs and district nurses, to ensure sick people receive more help with their convalescence after discharge and so are less likely to return to hospital. "Making hospitals responsible for a patient's ongoing care after discharge will create more joined-up working between hospitals and community services and may be supported by the developments in re-ablement and post-discharge support," he says.I hope in reading the above you have a sense of my frustration in that the health career model can encourage and support timely reflection that can help achieve holistic, integrated - coherent care.
- a common resource -
across disciplines and available to patients and carers
then the potential benefits (and savings?) are even greater.

 orcid.org/0000-0002-0192-8965
orcid.org/0000-0002-0192-8965