Conceptual Reflections on Schizophrenia - Hodges' model
A decade ago I was studying the Psychosocial Interventions for Psychosis (COPE) pathway part-time at Manchester University. The student body was interprofessinal made up of nurses, psychologists, occupational therapists, nurses and if memory serves me right people from the voluntary (third) sector. What I learned then left me wondering where I had been all those years since qualifying (lost in IT....).
There are many universities now delivering this curriculum, presenting the very latest research. The lecturers are frequently the researchers themselves, working in ongoing multicenter trials studying various aspects of the treatment and care management of psychosis.
This is why it is very alarming to hear of the lack of progress not just within in-patient care as per the findings of the Schizophrenia Commission, but the delivery of care for these individuals and their families across the health and social care system. Of course, as a former student and holder of a PG(Dip.) I am not at present practising these skills formally.
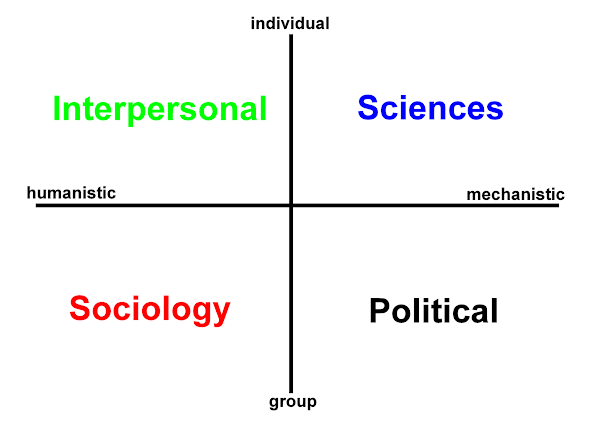
In the h2cm table that follows I have highlighted some of the main concepts across the care domains of Hodges' model:
| beliefs, perception, attention, anxiety, stress, vulnerability, pleasure, feedback, motivation, mood, therapies, therapeutic relationship, communication, assets, cognitive triad, perception, delusions, hallucinations, positive and negative symptoms, person-centered care, existing coping strategies, mental health assessment, literacies (3Rs, emotional, health), salience, attention, attribution, meaning, creativity | physical health, weight, fitness, side effects, medication, atypical antipsychotics, evidence, genetics, research, diagnosis, (cognitive) information processing, dual diagnosis, risk, models of care, recovery, hierarchy of clinical evidence, care processes - assessment, care planning, access to interventions, audio recording of sessions, protocols, DSM IV |
| clinical supervision, social attitudes - family, friends, community, stigma, myth, media, carers, familes, social relationships, network, self help groups, survivors, www.hearing-voices.org/ activities, daily routine, 'value' of a diagnosis - pros & cons (discuss), community centers, clinical supervision, positive risk management, employment, social history of mental health, social psychiatry, stories,education - schools & community, 'community care', housing | mental health history, institutional vs. community care, mental health law, autonomy, consent, capacity, best interests, equity mental health services, early intervention, access, POLICY, anti-psychiatry, equity, governance, data gathering, statistics, reporting, outcomes, services, secure provision, early intervention, crisis intervention, DSM V, commissioning, funding for mental health, education and training, sickness - welfare benefits - 'incapacity' review 'return to work' |
The relative position of concepts above does not indicate priority.

 orcid.org/0000-0002-0192-8965
orcid.org/0000-0002-0192-8965